NUCHAL TRANSLUCENCY / COMBINED TEST – OSCAR
Nuchal Translucency scan and Nasal Bone Scan : 11 – 13 weeks (First trimester)
- Whether you are definitely pregnant
- How many babies you are expecting
- How many weeks pregnant you are
- Whether there are any obvious major abnormalities present at this time
- The risk of chromosomal abnormalities, especially Down’s syndrome
- Examination of the fetal nose
- Examination of baby/fetal sex
At this gestation the fetus will be 2 – 3 inches (5 – 8cms) long and the heartbeat can be demonstrated on the screen. The “crown-rump” length will be measured and your expected date of delivery confirmed. Unfortunately, in about 3% of women who attend for this scan, it is found that the fetus has died, often several weeks before and without any warning. If this has happened appropriate arrangements will be made.
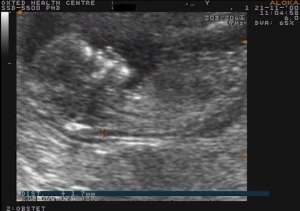
(Click Photo to Expand)
If the calculation gives you an increased risk, you may be happy to continue without further investigation or you may feel you want a more definite answer. In this case we can refer directly for an invasive test, (usually chorionic villus sampling), carried out at a specialist centre. The advantage of an invasive test is that you get a definite answer, the disadvantage is that the test carries a 1% risk of causing miscarriage. This will be fully discussed at the time of your scan.During the scan we will measure the amount of fluid at the back of your baby’s neck (Nuchal Translucency). Using this measurement, along with the mother’s age, the age of the baby and the presence or absence of the baby’s nasal bone, a risk is calculated to determine the likelihood of your baby having a chromosomal abnormality. 95% of measurements will indicate a reduced risk.
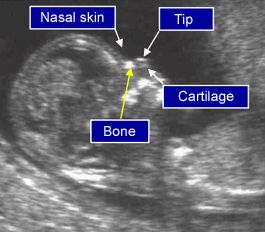
A blood test can be performed as an adjunct to the Nuchal and Nasal bone scan, as described above, which slightly increases the overall detection of Down’s syndrome screening. This is recommended by the National Down’s Syndrome Screening Committee.Combined Test (Nuchal Translucency, Nasal Bone and blood test – OSCAR)
The blood test performs better from 10 weeks gestation and the Nuchal scan performs best at 12 weeks gestation, although both tests can be done up to 14 weeks.
In order to get a one stop clinic with your results, (OSCAR), we recommend that you attend for the blood test prior to the scan.
If you are not certain whether you would like the blood test, the scan can be performed first, and if necessary, the blood taken after the scan.
If you are in doubt about which test you would like, the sonographer can discuss the issues in more detail with you prior to making a booking.
Trisomy 21 (Down’s syndrome) – Risk by maternal age and gestation:
– estimated risk (1/ number in this table)
| Age (years) | 12 weeks | Birth |
| 20 | 898 | 1527 |
| 22 | 872 | 1482 |
| 24 | 827 | 1406 |
| 26 | 756 | 1286 |
| 28 | 655 | 1113 |
| 30 | 526 | 895 |
| 31 | 457 | 776 |
| 32 | 388 | 659 |
| 33 | 322 | 547 |
| 34 | 262 | 446 |
| 35 | 210 | 356 |
| 36 | 165 | 280 |
| 37 | 128 | 218 |
| 38 | 98 | 167 |
| 39 | 75 | 128 |
| 40 | 57 | 97 |
| 41 | 43 | 73 |
| 42 | 32 | 55 |
| 43 | 24 | 41 |
| 44 | 18 | 30 |
Aid to pre-test counselling
- Performed at 11 – 13 weeks’ gestation
- Aimed at all pregnant women
- Individual risk prior to the test is determined by maternal age (See chart above)
- The test screens for those at increased risk of chromosomal abnormality – particularly Down’s syndrome
- The test is performed by either transabdominal or transvaginal ultrasound scan
- 95% of women tested will have a normal result
- Further testing is usually offered if the recalculated risk after nuchal translucency measurement is greater than 1:300
- The test will pick up 80% of pregnancies affected by Down’s syndrome – this compares with 60% picked up by serum screening (the triple test) and 30% when selected by age alone (35 years+)
- The test itself does not carry any risk to the mother or the baby
- If a test is positive (i.e. recalculated risk is greater than 1:300) an invasive test is usually recommended to determine the baby’s chromosomal pattern. This may be chorion villus sampling (CVS) -performed at 11 – 14 weeks – or amniocentesis performed at 16 weeks’ gestation. Both of these tests carry a risk of miscarriage of ~1%